What do you need to know about Alexander's Disease?
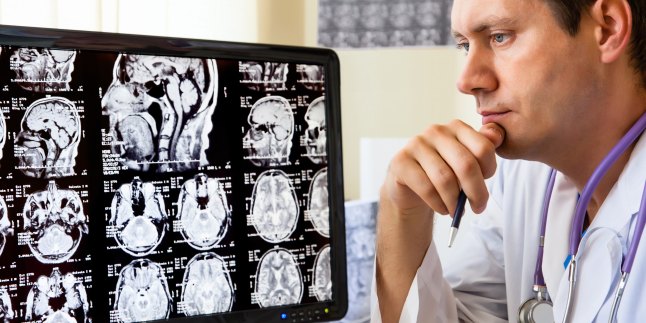
At first, four forms of Alexander's disease were described according to the age of onset: neonatal, infant, juvenile and adult. In time, however, more data has been obtained and this classification has been revised, the new one containing only two forms: Type I, with onset before 4 years, and Type II, with onset after age 4, the distribution being approximately . Symptoms associated with type I include: - growth retardation in height and weight, - delays in physical, mental and behavioral development (psychomotor developmental disorders), - macrocephaly, or increased head circumference, - muscle spasticity and restraining movements, - lack of . Approximately 90% of sick children have developmental problems and half have other symptoms. However, there is no symptom or combination of symptoms to be present in each case. Patients with type II rarely develop delays in development, macrocephaly or seizures, and cognitive decline installs extremely slowly or not at all.
They may show pseudobulbar or bulbous signs (in half of cases), 75% have ataxia and 33% spasticity. Because the symptoms are not specific, the adult form of Alexander's disease is confused often confused with or with neoplastic processes. Comorbidities: - hypotonia - - - hypertension - - early puberty - scoliosis, lordosis or - mood disorders - osteopenia. Approximately 95% of cases are caused by gene mutations, called GFAP. This gene is involved in the production of a structural protein, called the glial fibrillar acid protein, located on chromosome 17.
Mutations determine alteration of protein structure and its accumulation in astrocytes, thus constituting Rosenthal fibers. There is still no knowledge of the remaining 5 percent remaining. Alexander's disease is an autosomal dominant disease, which means that a single copy of a mutant gene is required to develop the disease. Most patients acquire new mutations, indicating that none of the parents had that mutation. However, the mutation may occur during sperm or egg development.
The risk of transmission of this genetic disease is 50% for each pregnancy. Diagnosis is usually established by a neurologist or pediatric neurologist. Of course, for a complete diagnosis and effective disease management, a multidisciplinary team involved in each case. Perform a complete neurological examination, an assessment of age-specific development, and note the presence of certain disorders such as eating disorders, nutritional deficits, growth disorder. Psychological assessments, family structure, social assessments, genetic or orthopedic advice can also be made.
Paraclinic examinations, which provide more information about pathophysiology of the disease, are cerebral MRI, (EEG), lumbar puncture, or histopathological examination. Thus, changes in the MRI may occur on the MRI, especially in the frontal lobes, but also in other areas such as the ventricular brain system, basal ganglion or thalamus. For newborns, the most common lesions appear in the frontal lobes and basal ganglia, and adults show several changes in the cerebral trunk. On the EEG, there will be observed slow waves in the frontal cerebral areas, and in the case of epileptiform discharges. Lumbar puncture, along with CSF analysis, will highlight elevated levels of fibrous acid glial protein or other protein accumulations.
The histopathological examination of cerebral biopsy was the reference exam for the diagnosis of certainty in Alexander's disease, but recent advances in imaging place the MRI test first in the diagnosis of this disease, especially for type I. Because type II does not show white matter damage, abnormalities in the cerebral cortex, cerebellum and spinal cord suggest the diagnosis. A definitive diagnosis is only established after identifying the GFAP mutation in the patient's DNA. However, there are 5 percent that do not present this mutation, and a negative result does not rule out the diagnosis. Unfortunately, for people with Alexander disease who do not have the GFAP mutation, the diagnosis of certainty is established only after autopsy, where the presence of disseminated Rosenthal fibers.
To diagnose Alzheimer's disease properly, other diseases that have a similar presentation must be eliminated, such as: • Other Leucodistrophies: Krebbe's leukodystrophy • Zellweger's syndrome • Glutaric acid and hydroxyglutaric acid • Tay-Sachs disease • Pelizaeus-Merzbacher disease . Treatment Unfortunately, no curative treatment for Alexander's disease has yet been found. The only treatments that can be done are symptomatic and prevent complications. Genetic counseling is essential if one of the parents suffers from Alexander's disease or a family history. Prenatal genetic testing for pathogenic variants of the GFAP gene may also be an option.
Source : sfatulmedicului.ro
Views : 2945
Popular Article
- (photo) Nude becomes art.
Posted: 2018-03-17, 9587 views.
- The harmful effects of air conditioning on the skin
Posted: 2017-06-08, 8267 views.
- 3 causes of dyed hair discoloration
Posted: 2017-06-15, 8140 views.
- Why early puberty occurs in girls: symptoms, favors, diagnosis and treatment
Posted: 2017-10-24, 7996 views.
- Good or bad skin treatments in the hot season
Posted: 2017-06-07, 7736 views.
Recommendations
- (photo) Nude becomes art.
Posted: 2018-03-17, 9587 views.
- The harmful effects of air conditioning on the skin
Posted: 2017-06-08, 8267 views.
- 3 causes of dyed hair discoloration
Posted: 2017-06-15, 8140 views.
- Good or bad skin treatments in the hot season
Posted: 2017-06-07, 7736 views.
- Risks of practicing sports on hot days
Posted: 2017-06-12, 7328 views.
 4 effective ingredients in the fight against acne.
4 effective ingredients in the fight against acne. How to get rid of hiccups fast
How to get rid of hiccups fast The wheat bran diet: the secret of lost pounds as if by magic
The wheat bran diet: the secret of lost pounds as if by magic The recipe that will sweeten your soul this weekend!
The recipe that will sweeten your soul this weekend!  Is it dangerous or not to refreeze meat after thawing it?
Is it dangerous or not to refreeze meat after thawing it?  The unusual sign of diabetes indicated by saliva.
The unusual sign of diabetes indicated by saliva. What to drink to boost your immune system.
What to drink to boost your immune system. 10 foods that help you never age.
10 foods that help you never age. What actually happens in your body if you drink a cup of coffee for breakfast
What actually happens in your body if you drink a cup of coffee for breakfast 5 surprising benefits of chia seeds
5 surprising benefits of chia seeds